Antidiabetic drugs, also known as glucose-lowering medications, are a class of drugs used to treat type 1 and type 2 diabetes mellitus. They work by reducing blood sugar levels through various mechanisms, such as increasing insulin production, reducing glucose absorption, or enhancing insulin sensitivity. Examples of antidiabetic drugs include metformin, sulfonylureas, thiazolidinediones, and DPP-4 inhibitors.
These drugs play a crucial role in managing diabetes by helping to control blood sugar levels and prevent complications such as heart disease, kidney disease, and blindness. The choice of antidiabetic drug depends on the type of diabetes, disease severity, and individual patient factors. Regular monitoring of blood sugar levels and lifestyle modifications, including diet and exercise, are essential for effective diabetes management.
The development and use of antidiabetic drugs have revolutionized diabetes care, significantly improving the quality of life for people with this condition. Ongoing research continues to explore new and improved treatments to further enhance diabetes management and prevent complications.
Antidiabetic Drugs
Antidiabetic drugs, also known as glucose-lowering medications, play a critical role in managing diabetes mellitus. Their primary function is to reduce blood sugar levels through various mechanisms. Here are seven key aspects related to antidiabetic drugs:
- Mechanism of Action: Drugs like metformin increase insulin sensitivity, while sulfonylureas stimulate insulin release.
- Types: Antidiabetic drugs include several classes, such as biguanides, sulfonylureas, thiazolidinediones, and DPP-4 inhibitors.
- Indications: These drugs are used to treat both type 1 and type 2 diabetes mellitus.
- Combination Therapies: Often, combinations of antidiabetic drugs are used to achieve optimal blood sugar control.
- Monitoring: Regular monitoring of blood sugar levels is essential while taking antidiabetic drugs.
- Lifestyle Modifications: Antidiabetic drugs are most effective when combined with healthy lifestyle choices, including diet and exercise.
- Research and Development: Ongoing research aims to improve the efficacy and safety of antidiabetic drugs.
In conclusion, antidiabetic drugs are essential for managing diabetes mellitus, helping to control blood sugar levels and prevent complications. The choice of drug depends on the type of diabetes, individual patient factors, and disease severity. Regular monitoring, lifestyle modifications, and ongoing research are crucial for effective diabetes management and improved patient outcomes.
Mechanism of Action
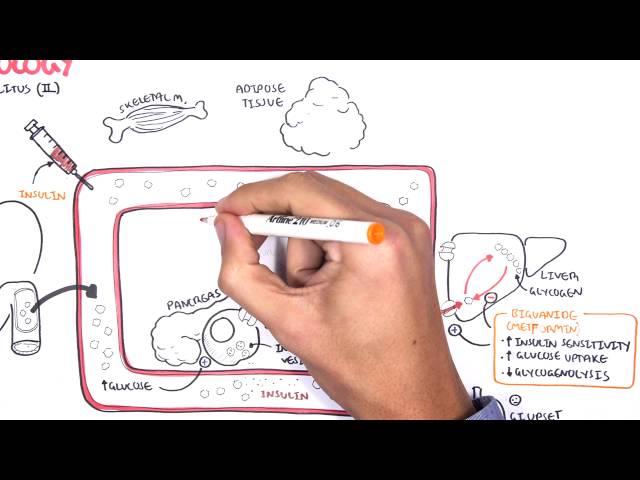
Understanding the mechanism of action of antidiabetic drugs is crucial for optimizing their use in managing diabetes mellitus. Metformin, a commonly prescribed antidiabetic drug, works by increasing insulin sensitivity, particularly in the liver and skeletal muscle. This enhanced sensitivity allows the body’s cells to take up and utilize glucose more effectively, leading to a reduction in blood sugar levels.
On the other hand, sulfonylureas, another class of antidiabetic drugs, stimulate insulin release from the pancreas. Insulin is a hormone that promotes glucose uptake by cells, thereby lowering blood sugar levels. Sulfonylureas are particularly effective in individuals with type 2 diabetes who still have some functioning beta cells in their pancreas.
The choice of antidiabetic drug depends on several factors, including the type of diabetes, disease severity, and individual patient characteristics. Understanding the mechanism of action of different drugs enables healthcare providers to tailor treatment plans to achieve optimal blood sugar control and improve patient outcomes.
Types
Antidiabetic drugs are classified into several groups based on their mechanism of action. These classes include biguanides, sulfonylureas, thiazolidinediones, and DPP-4 inhibitors, each with unique characteristics and effects on blood sugar control.
The classification of antidiabetic drugs is crucial for understanding their appropriate use and optimizing therapeutic outcomes. Different classes of drugs target specific aspects of glucose metabolism, allowing healthcare providers to tailor treatment plans to individual patient needs.
For instance, biguanides like metformin are often first-line agents for managing type 2 diabetes due to their ability to improve insulin sensitivity and reduce hepatic glucose production. Sulfonylureas, on the other hand, stimulate insulin secretion from the pancreas, making them particularly effective in individuals with type 2 diabetes who still have functioning beta cells.
Understanding the different classes of antidiabetic drugs and their mechanisms of action is essential for healthcare providers to make informed decisions about drug selection, dosage, and combination therapies. This knowledge empowers them to provide personalized and effective diabetes management, ultimately improving patient outcomes and quality of life.
Indications
Antidiabetic drugs play a vital role in the management of both type 1 and type 2 diabetes mellitus, addressing the specific challenges and characteristics of each type.
- Type 1 Diabetes: In type 1 diabetes, the body’s immune system attacks and destroys the insulin-producing beta cells in the pancreas, leading to an absolute deficiency of insulin. Antidiabetic drugs, particularly insulin replacement therapy, are essential for managing type 1 diabetes, as the body can no longer produce its own insulin.
- Type 2 Diabetes: In type 2 diabetes, the body develops insulin resistance, meaning that the cells do not respond effectively to insulin, and/or there is a relative deficiency of insulin. Antidiabetic drugs can help improve insulin sensitivity, increase insulin secretion, or both, depending on the specific medication and the individual patient’s needs.
The use of antidiabetic drugs in both type 1 and type 2 diabetes mellitus underscores their versatility and importance in managing this chronic condition. These drugs help control blood sugar levels, reduce the risk of complications, and improve overall health outcomes for people with diabetes.
Combination Therapies
Combination therapies, involving the use of multiple antidiabetic drugs, play a crucial role in achieving optimal blood sugar control, particularly in individuals with complex or advanced diabetes management needs.
The rationale behind combination therapies lies in targeting different mechanisms of action. By combining drugs with complementary effects, healthcare providers can address various aspects of glucose metabolism and maximize therapeutic outcomes. For instance, combining metformin, which enhances insulin sensitivity, with a sulfonylurea, which stimulates insulin secretion, can provide a more comprehensive approach to managing blood sugar levels.
Combination therapies also allow for personalized treatment plans, tailoring drug combinations to individual patient characteristics and response to therapy. This approach enables healthcare providers to optimize blood sugar control, reduce the risk of complications, and improve overall health outcomes for people with diabetes.
The use of combination therapies highlights the versatility and adaptability of antidiabetic drugs in managing diabetes. By leveraging the synergistic effects of different medications, healthcare providers can effectively address the complex challenges of diabetes management and improve the quality of life for people living with this condition.
Monitoring
Regular monitoring of blood sugar levels is an indispensable component of effective antidiabetic drug therapy. Here’s why:
- Assessing Treatment Efficacy: Blood sugar monitoring helps healthcare providers evaluate the effectiveness of antidiabetic drugs and adjust dosages or treatment plans as needed. This ensures optimal blood sugar control and reduces the risk of complications.
- Hypoglycemia Prevention: Some antidiabetic drugs, particularly insulin and sulfonylureas, can cause hypoglycemia (low blood sugar). Regular monitoring allows individuals to detect and promptly treat hypoglycemia, preventing its potentially serious consequences.
- Medication Adjustment: Blood sugar monitoring provides valuable information for healthcare providers to make informed decisions about medication adjustments. Based on monitoring results, they can increase or decrease dosages, add or remove medications, or switch to alternative therapies to achieve optimal glycemic control.
In summary, regular blood sugar monitoring is crucial for the safe and effective use of antidiabetic drugs. It empowers individuals to take an active role in managing their diabetes, preventing complications, and improving their overall health outcomes.
Lifestyle Modifications
Lifestyle modifications are a cornerstone of effective diabetes management, and they play a crucial role in enhancing the efficacy of antidiabetic drugs. A healthy lifestyle, encompassing a balanced diet and regular physical activity, offers numerous benefits that complement and optimize drug therapy for individuals with diabetes.
- Improved Blood Sugar Control: A balanced diet, rich in fruits, vegetables, and whole grains, helps maintain stable blood sugar levels. Regular exercise increases insulin sensitivity, allowing the body to utilize glucose more effectively, leading to improved glycemic control.
- Reduced Medication Dependence: Lifestyle modifications can reduce the reliance on antidiabetic drugs. Diet and exercise can improve insulin sensitivity and glucose metabolism, potentially allowing for lower medication dosages or even discontinuation in some cases.
- Prevention of Complications: A healthy lifestyle helps prevent the development and progression of diabetes-related complications, such as heart disease, stroke, and kidney disease. Regular physical activity and a balanced diet promote overall cardiovascular health, reduce blood pressure, and improve lipid profiles.
- Enhanced Quality of Life: Lifestyle modifications contribute to an improved quality of life for individuals with diabetes. Regular exercise boosts energy levels, improves mood, and reduces stress. A nutritious diet provides essential vitamins and minerals, promoting overall well-being.
In summary, lifestyle modifications are indispensable for effective diabetes management in conjunction with antidiabetic drugs. By adopting a healthy diet and engaging in regular physical activity, individuals with diabetes can optimize blood sugar control, reduce medication dependence, prevent complications, and enhance their overall quality of life.
Research and Development
Ongoing research and development in antidiabetic drugs are crucial for improving the lives of individuals with diabetes. Pharmaceutical companies and research institutions are continuously exploring new avenues to enhance the efficacy and safety of these medications, leading to better outcomes for patients.
Research efforts focus on addressing unmet medical needs, such as developing drugs with improved glucose-lowering capabilities, reduced side effects, and more convenient administration methods. The ultimate goal is to provide patients with diabetes with effective and well-tolerated treatment options that enable them to manage their condition effectively and maintain a good quality of life.
The development of new antidiabetic drugs involves rigorous research processes, including preclinical studies in animal models and clinical trials in human participants. These trials evaluate the safety and efficacy of new drugs, comparing them to existing treatments and assessing their potential benefits and risks. Through ongoing research and development, the field of diabetes management continues to advance, bringing hope and improved outcomes for individuals living with this condition.
FAQs on Antidiabetic Drugs
This section provides answers to frequently asked questions about antidiabetic drugs, addressing common concerns and misconceptions.
Question 1: What are antidiabetic drugs, and how do they work?
Answer: Antidiabetic drugs are medications used to lower blood sugar levels in individuals with diabetes. They work through various mechanisms, such as increasing insulin production, enhancing insulin sensitivity, or reducing glucose absorption.
Question 2: Are antidiabetic drugs safe for long-term use?
Answer: The safety of antidiabetic drugs depends on the specific medication and individual patient factors. Generally, these drugs are considered safe for long-term use when taken as prescribed and under the supervision of a healthcare provider.
Question 3: Can antidiabetic drugs cause side effects?
Answer: Yes, antidiabetic drugs can cause side effects, but the type and severity vary depending on the medication. Common side effects include nausea, diarrhea, weight gain, and hypoglycemia (low blood sugar).
Question 4: How are antidiabetic drugs typically taken?
Answer: Antidiabetic drugs can be taken orally, injected, or administered through an insulin pump. The specific method of administration depends on the type of medication and individual patient needs.
Question 5: Is it possible to manage diabetes without antidiabetic drugs?
Answer: In some cases, it may be possible to manage diabetes through lifestyle modifications alone, such as diet, exercise, and weight loss. However, for many individuals, antidiabetic drugs are necessary to achieve and maintain optimal blood sugar control.
Question 6: Are there any new developments in antidiabetic drug research?
Answer: Yes, ongoing research is focused on developing new antidiabetic drugs with improved efficacy, reduced side effects, and more convenient administration methods. These advancements aim to provide better treatment options for individuals with diabetes.
Summary: Antidiabetic drugs play a crucial role in managing diabetes by lowering blood sugar levels. They are generally safe for long-term use, but potential side effects should be discussed with a healthcare provider. Ongoing research continues to improve the efficacy and safety of these medications, leading to better outcomes for individuals with diabetes.
Transition to the Next Section: For more detailed information on specific antidiabetic drugs, their mechanisms of action, and treatment guidelines, please refer to the following section.
Tips for Managing Diabetes with Antidiabetic Drugs
Antidiabetic drugs can effectively lower blood sugar levels and improve overall health outcomes for individuals with diabetes. To optimize the use of these medications, consider the following tips:
Tip 1: Adhere to Prescribed Regimen
Take antidiabetic drugs exactly as prescribed by your healthcare provider, including the correct dosage, frequency, and timing. Skipping or altering doses can compromise blood sugar control.
Tip 2: Monitor Blood Sugar Regularly
Regular blood sugar monitoring is crucial to assess the effectiveness of antidiabetic drugs and to detect and manage blood sugar fluctuations. Follow your healthcare provider’s instructions for monitoring frequency.
Tip 3: Engage in Regular Physical Activity
Exercise improves insulin sensitivity and helps control blood sugar levels. Aim for at least 30 minutes of moderate-intensity exercise most days of the week.
Tip 4: Maintain a Balanced Diet
Choose a diet rich in fruits, vegetables, and whole grains. Limit processed foods, sugary drinks, and unhealthy fats to support healthy blood sugar levels.
Tip 5: Manage Stress
Stress can elevate blood sugar levels. Practice stress-reducing techniques such as yoga, meditation, or deep breathing exercises to help manage stress and improve diabetes control.
Tip 6: Get Adequate Sleep
Sleep deprivation can impair insulin sensitivity. Aim for 7-9 hours of quality sleep each night to support optimal blood sugar management.
Tip 7: Avoid Smoking and Limit Alcohol
Smoking and excessive alcohol consumption can interfere with blood sugar control. Quit smoking and limit alcohol intake to improve overall health and diabetes management.
Summary: By following these tips and working closely with your healthcare provider, you can effectively manage diabetes with antidiabetic drugs. Adherence, monitoring, lifestyle modifications, and stress management are key factors in achieving and maintaining optimal blood sugar control.
Transition to the Conclusion: To further enhance your understanding of antidiabetic drugs and their role in diabetes management, explore the following resources and consult with your healthcare provider for personalized guidance.
Conclusion
Antidiabetic drugs play a vital role in the management of diabetes, helping to control blood sugar levels and prevent complications. These medications work through various mechanisms, including increasing insulin production, enhancing insulin sensitivity, or reducing glucose absorption. Healthcare providers carefully select and combine antidiabetic drugs based on individual patient needs and disease severity to achieve optimal glycemic control.
Lifestyle modifications, such as maintaining a healthy diet, engaging in regular physical activity, and managing stress, are crucial complements to antidiabetic drug therapy. By adopting these healthy habits, individuals with diabetes can further improve their blood sugar control and overall well-being.
Ongoing research and development in antidiabetic drugs continue to focus on improving efficacy, safety, and convenience. These advancements hold promise for better diabetes management outcomes, empowering individuals to live healthier and more fulfilling lives.
Youtube Video: